How
The main goals of the pilot was to analyze antenatal women's willingness to pay for an ultrasound, to examine the ability of midwives to become social entrepreneurs, and to test the viability of the proposed business case. To this end, the following intervention and activities were conducted:
- The project was fully aligned with and endorsed by key stakeholders, including the Society of Radiography in Kenya, the Nursing Council of Kenya, the Midwives Association of Kenya, and the County Governments.
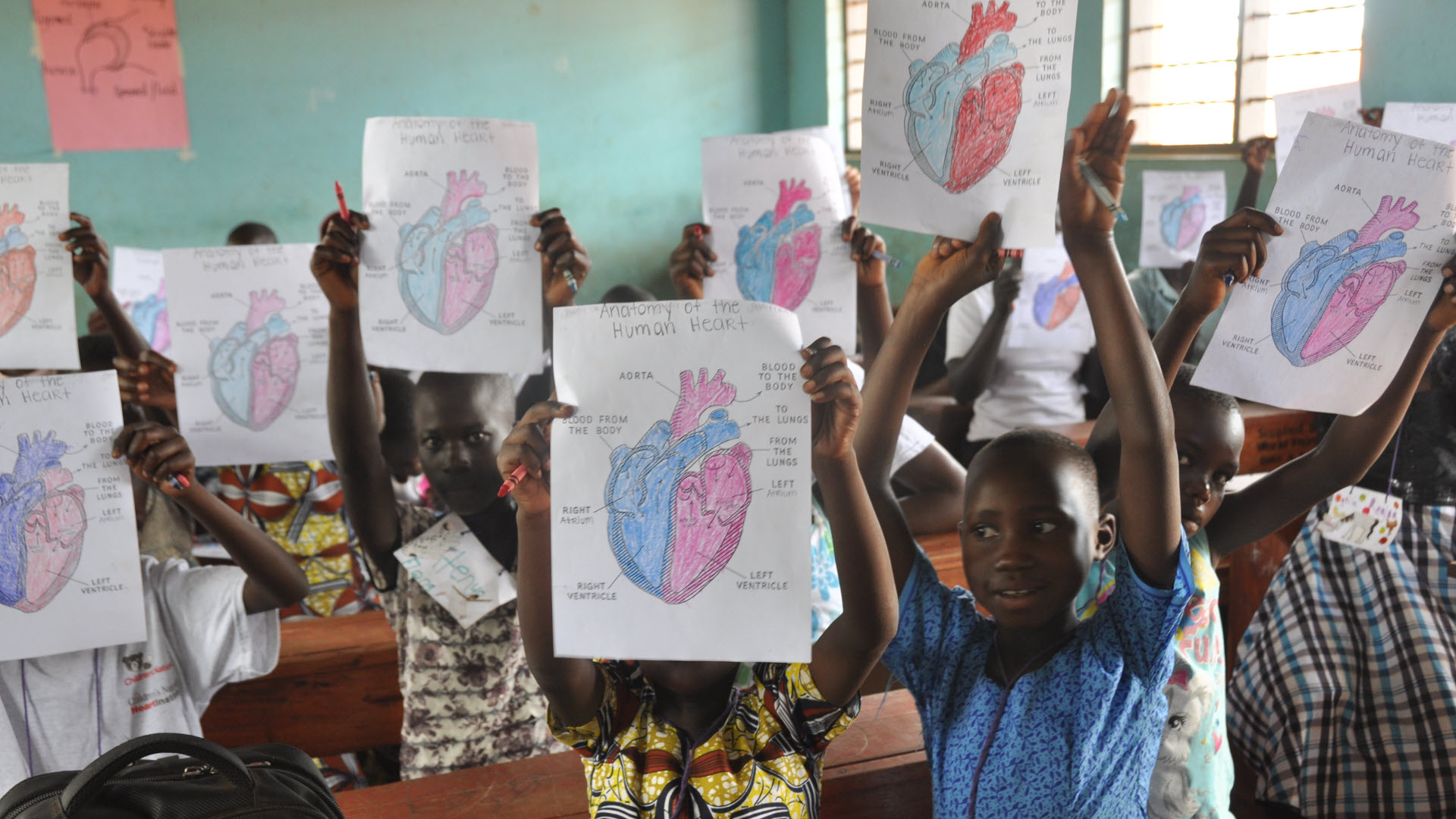
- 42 midwives were trained successfully on two standardized and blended learning modules. 10 sonographers were involved in the training, and subsequently supported the midwives in conducting and interpreting the screenings. 950 pregnant women were screened for free during this training. To date, a total of 67 midwives have been trained. The ability of midwives to correctly conduct obstetric ultrasound screening was assessed and rated by radiologists.
- 2-5 midwives were grouped into business units (BUs) to create functional teams in 10 health facilities in 2 counties in Kenya (Kadjiado and Kisii). Each business unit was mentored by a radiographer. Each business unit received a point-of-care ultrasound device, and a connection to a digital platform which enabled remote collaboration with professional sonographers. County governments allowed the midwives to charge KSh500 per session. Midwives’ monthly incentive was performance based.
- The study identified women’s motivations and barriers to take up routine ultrasound screening and their willingness to pay for it.
Based on these findings, the study explored a potential income model for midwives.